Cardiac catheterisation is known as the ‘gold standard’ test to diagnose pulmonary hypertension. It is a procedure that is used to study the right side of the heart and it is also referred to as a right heart catheter, or RHC.
Cardiac catheterisation can provide accurate information about the blood pressure in the heart and pulmonary artery. It involves a small tube (catheter) being passed into a vein and guided around your body to take measurements in the heart and lungs.
Dr Charlie Elliott of the Sheffield Pulmonary Vascular Disease Unit has performed hundreds of these procedures. In the video below, he explains more about them. Underneath, you’ll find answers to common questions.
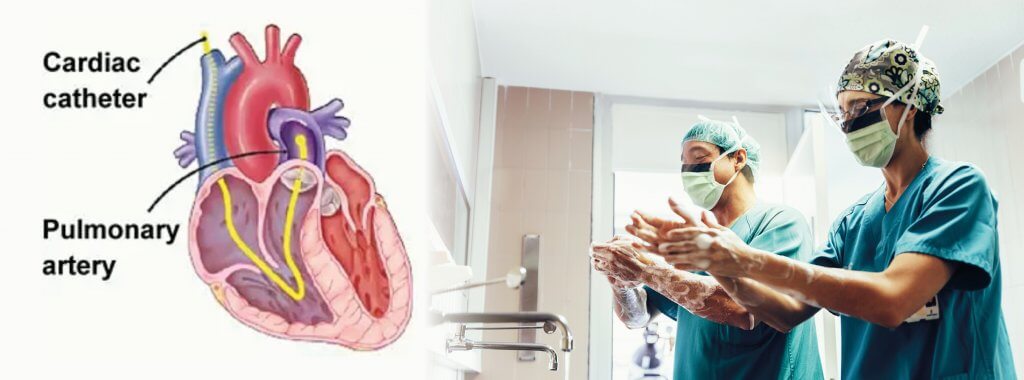
Cardiac catheterisation is the most accurate way to measure the blood pressure in your heart and the blood vessels in your lungs (the pulmonary arteries). Along with other tests, this will help your doctor to tell whether you have pulmonary hypertension or if your symptoms are caused by something else. It may also help guide the best treatment for you so it can be a very important test.
It is usually performed by a cardiologist (heart specialist) or a respiratory physician (lung specialist) and is done in the hospital. During the procedure, the doctor uses local anaesthetic and inserts a very thin, flexible tube (catheter) into a vein in your body and guides it to your heart. The catheter allows the doctor to record measurements in the heart and the blood vessels in the lungs.
The pressure inside the chambers of your heart and the blood vessels in your lungs is measured, along with the oxygen levels in the blood. The procedure also works out how much blood the heart is pumping.
This section describes the important measurements taken using cardiac catheterisation.
The procedure is usually performed in a specially equipped room in the hospital called the cardiac catheterisation laboratory (sometimes cath lab for short). Exactly where it is will depend on the hospital and your specialist team will be able to tell you more.
The procedure usually takes less than an hour. Most people can go home the same day but it’s possible (although rare) that you may need to stay in the hospital overnight.
Before going to the cath lab a doctor will talk to you about the procedure. They will answer your questions and provide any further information if needed to be sure you understand everything. You will then be asked to sign a consent form.
You will be given a hospital gown to change into and then you will be taken to the cath lab. Once there, you will be transferred to a special table that x-rays can be taken through. You will need to lay fairly flat throughout the procedure. Let the team know beforehand if you have back or breathing problems that may make this difficult for you. You need to be awake during the procedure so that you can follow instructions so you may not be given sedative medication before the catheterisation.
A doctor or staff member will prepare an entry point for the catheter, usually at the neck or upper thigh (groin). The area will be cleaned, possibly shaved, and then numbed with local anaesthetic. You should not experience much discomfort apart from the initial sting of the local anaesthetic injection. If you do experience any discomfort or there is anything that is worrying you about the test you should let the team know straight away so that they can help.
Once the local anaesthetic has been applied, the doctor makes an opening in the vein and threads in a long, thin, flexible tube, called a catheter into the vein. They then direct the catheter along the vein, through the heart and into the blood vessels in the lungs. An x-ray machine and other equipment is used to monitor the position of the catheter.
The catheter is used to measure the pressure in the heart and in the blood vessels in the lung. They also record how much oxygen is in your blood and the amount of blood your heart is pumping each minute.
A vasodilator challenge may be done during the procedure. This can help guide your treatment. It involves giving a short-acting medication (often something that can be breathed in from a mask) to see if the pressurein your lungs falls in response to that particular medication.
A ‘fluid challenge’ might be given at the time of the procedure. This is to see how the heart copes with a little extra fluid and can help work out why the pressure is high in the lungs.
You may be asked to undertake some form of exercise during the procedure. This is to see how the heart and the pressure responds to working a bit harder than when resting. It may involve turning the pedals of a special exercise bike during the test and can give a bit more information about how the heart and lungs work together.
Once all the measurements have been completed, the catheter is carefully removed and the doctor will apply pressure to the small puncture site to prevent bleeding. After this, a dressing is placed over the entry site, and you will be taken to a recovery room.
Please follow any instructions you have been given and let the staff know if you have an allergy or sensitivity to any medications, latex etc.
No fasting is required and you should take your medications as normal unless instructed otherwise by your doctor. Wear loose comfortable clothing and shoes.
If possible, come with a family member or friend who can accompany you home. It is generally recommended that you don’t drive home after the tests if possible. You can be tired and rarely a bit sore for the evening after the procedure so having someone to drive you home or other transport would be preferred.
Your specialist team may tell you to stop taking certain medications around the time of the procedure. This will most often relate to blood thinning medication (such as warfarin, rivaroxaban, apixaban or similar drugs) and specific instructions will be given to you about this and also restarting the medication after the test. You will see a doctor before you have your catheter and have the opportunity to ask any questions you have about the day, or your tests, before being asked to sign a consent form to show you agree to the test and understand what is involved.
You will be seen by a doctor after the procedure. They will be able to give you the preliminary results of your tests and if appropriate, possibly new medication before you go home.
Avoid heavy lifting for 24 hours. Things like coughing, sneezing or bending over can cause the site to bleed a little, so applying support to the puncture site if needed can help.
If you experience swelling, increased pain or bleeding after you leave hospital, you should apply direct pressure to the site and seek assistance from your local doctor or emergency department.
You should rest for the day of your procedure. The doctor will be able to advise you when you may be able to return to normal activities or work (which will depend on what that involves).
Most people undergo RHC without any problems, however, there are risks associated with any medical procedure. The risks associated with RHC are listed here for your information. A doctor will also discuss these risks with you before the RHC, answer any questions you have, providing any further information if needed to be sure you understand everything. Only then will you be asked to sign a consent form.
Common
(less than 1 in 20)
• Minor bleeding and bruising at the site of catheter insertion.
• Abnormal heart beat lasting several seconds that settles by itself.
• Difficulty passing the catheter into the neck vein.
• Flushed hot feeling that settles quickly.
• Back pain related to lying flat.
Rare
(less than 1 in 500)
• Local anaesthetic around your voice box may cause temporary loss of voice – this wears off quickly.
• Abnormal Heart Rhythm that continues for a longer time and may need treatment either to slow down a fast heart beat or speed up a slow one.
• Punctured artery in the neck that may cause bruising or bleeding and require repair.
• Allergic reaction.
• Air entering the vein and lodging in the lung.
• Collapsed lung.
Extremely rare
(less than 1 in 1000)
• Life threatening damage to the lung blood vessels.
• Stroke.
• Infection.
• Death.
It’s best to talk to the doctor at the time they suggest the procedure in the first place if you have any concerns.
If you only think about it later, let the medical team know as soon as possible. They will be able to explain why they the think the test is necessary. This is usually because it will be able to measure the pressure in your lungs and other things that can sometimes only be estimated by other tests. It is the results of all these tests together that help decide if treatment should be given and which sort.
If a right heart catheter is not done the doctor will not have all the information they might require and will need to make the best decision they can with the information available to them. This increases the risk of you receiving treatment that might not help you or might not be the best type. This can be very different from person to person, so it is best to talk to one of the team about your concerns as soon as possible.